Cancer Care
-
Prostate Cancer
-
Bladder Cancer
-
Kidney Cancer
-
Testicular Cancer
<
>
Prostate Cancer
Prostate cancer is the #1 most common cancer among men aside from skin cancer. Every year more than 1 million men are diagnosed with prostate cancer worldwide (accounting for 15% of all new cancers diagnosed in men), and 300,000 die from the disease.
Jamaica has one of the highest rates of newly diagnosed cases in the world ( 78.1/100 000/ year) ¹, which easily makes it the leading cancer affecting men in Jamaica. It is also the leading cause of male cancer-related deaths here at 53. 9 deaths/ 100 000/year ².
In general, the earlier the cancer is caught, the more likely it is for the patient be cured. Approximately 90% of all prostate cancers are detected in the early stages, before they cause symptoms, and so the cure rate for prostate cancer is very high. Some 70% to 100% of men diagnosed at this early stage will be disease-free five years after a curative procedure.
Every year we are discovering more about what causes prostate cancer. What scientists do know is that there are probably many reasons the disease occurs. These risk factors include:
It’s important to understand that by the time prostate cancer symptoms usually appear, the cancer is likely in a later stage and is generally not curable. The disease needs to be found and cured before symptoms develop, which is why prostate cancer screenings are recommended starting at age 40.
Men with early-stage prostate cancer may not have symptoms at all. In fact, it could be 10 years before symptoms become noticeable, and some older men may never have symptoms in their lifetime. In addition, other non-cancerous conditions of the prostate, such as Benign Prostatic Hyperplasia, or BPH, cause symptoms similar to Prostate cancer. This highlights the importance of getting tested before the onset of symptoms, which are mostly unreliable.
Some symptoms of prostate cancer may include:
Prostate Cancer Treatments
Prostate cancer treatment depends on the age and health of the patient, the aggressiveness of the cancer and the extent of the cancer at the time of diagnosis. Depending on stage of cancer, it may be cured with comparable efficacy by either surgery or radiation. However, all treatments for prostate cancer except observation may have significant side effects which affect the quality of life; urinary control, erectile function and bowel function are the primary concerns. For this reason, we believe in having a thorough discussion with you to weigh the risks and benefits of each option.
Active Surveillance: Some forms of the disease may grow so slowly that they don’t pose a risk to your health and require no treatment at all. The objective for these indolent or slow cancers is to offer close surveillance instead of a curative intent, thereby avoiding the problems associated with treatment. Should the cancer show signs of progression, intervention is offered while the cancer is still curable; there is significant progression in only 27% of these indolent cancers. This may also be a good choice for a man with a longer life expectancy who has a low-risk tumor.
Radiation Therapy: There are two types: interstitial prostate brachytherapy and external beam radiation therapy. With interstitial prostate brachytherapy, small radioactive “seeds” are planted in the prostate. With external beam radiation therapy, the prostate is treated from externally with a beam of radiation. The advantage of radiation therapy is that it is less invasive than surgery. Urinary control may be affected less often after radiation than with radical prostatectomy; however, bowel function can be adversely affected after radiation but not so for surgery. For very aggressive diseases, surgery followed by radiation therapy may be the best chance for a cure. However, one disadvantage of radiation therapy is that surgery cannot be performed afterwards if there is a recurrence.
Surgery: A radical prostatectomy is the standard of care for removal of the entire prostate and accessory glands. This surgery offers the man with cancer that has not spread outside the prostate an excellent chance of cure of his disease; depending on the aggressiveness of cancer, the cure rate may be as high as 95%. The most common side effects are erectile dysfunction and impaired urinary control. The chance of having erectile dysfunction depends on a man’s age and health, his sexual function before treatment and the stage of the cancer. Even if erectile dysfunction does occur after surgery, erections may return to normal over time, and can be improved on with medical therapy. While many men experience some form of urinary incontinence following prostate cancer treatment, the vast majority do regain their continence within a year. We can also recommend physiotherapy to assist with urinary function recovery, or pre-operatively to improve the after-surgery outcomes.
Hormone Therapy:This involves either stopping your body from producing the male sex hormone testosterone which stimulates the growth of prostate cancer cells, or blocking testosterone from getting into the cancer cells. Sometimes a combination of two drugs is used to achieve both effects. Hormonal therapy is offered to men who choose not to have, or who cannot be treated with, curative therapies.
--
1. Aiken WD, Tulloch T, Freeman V, Bennett F, Coard K, Panton B et al. Differences in patient characteristics in black men with prostate cancer from Jamaica and Chicago. In: Proc Am Soc Clin Oncol 2003; 22: (abstr 1764).
2. Blake G, Hanchard B, Mitchell K, Waugh N, Wolff C, Samuels E. Jamaica Cancer Mortality Statistics, 1999. West Indian Med J 2002; 51: 64−7
Jamaica has one of the highest rates of newly diagnosed cases in the world ( 78.1/100 000/ year) ¹, which easily makes it the leading cancer affecting men in Jamaica. It is also the leading cause of male cancer-related deaths here at 53. 9 deaths/ 100 000/year ².
In general, the earlier the cancer is caught, the more likely it is for the patient be cured. Approximately 90% of all prostate cancers are detected in the early stages, before they cause symptoms, and so the cure rate for prostate cancer is very high. Some 70% to 100% of men diagnosed at this early stage will be disease-free five years after a curative procedure.
Every year we are discovering more about what causes prostate cancer. What scientists do know is that there are probably many reasons the disease occurs. These risk factors include:
- Age: The diagnosis of prostate cancer is rare in men younger than 40. As men age, they are increasingly more likely to develop it. 1 in 6 men will be diagnosed in their lifetimes.
- Family history: If your father, grandfather, brother, son or other closely related family member has had prostate cancer, you are at an increased risk yourself.
- Race: Black men are 60% more likely to develop prostate cancer than Caucasian or Hispanic men.
It’s important to understand that by the time prostate cancer symptoms usually appear, the cancer is likely in a later stage and is generally not curable. The disease needs to be found and cured before symptoms develop, which is why prostate cancer screenings are recommended starting at age 40.
Men with early-stage prostate cancer may not have symptoms at all. In fact, it could be 10 years before symptoms become noticeable, and some older men may never have symptoms in their lifetime. In addition, other non-cancerous conditions of the prostate, such as Benign Prostatic Hyperplasia, or BPH, cause symptoms similar to Prostate cancer. This highlights the importance of getting tested before the onset of symptoms, which are mostly unreliable.
Some symptoms of prostate cancer may include:
- Difficulty urinating and/or difficulty starting and stopping urine flow
- Needing to urinate frequently, especially at night
- Pain or burning during urination
- Dull lower pelvic pain
- Blood in the urine or semen
- Painful ejaculation
- Pain in the lower back, hips or thighs
Prostate Cancer Treatments
Prostate cancer treatment depends on the age and health of the patient, the aggressiveness of the cancer and the extent of the cancer at the time of diagnosis. Depending on stage of cancer, it may be cured with comparable efficacy by either surgery or radiation. However, all treatments for prostate cancer except observation may have significant side effects which affect the quality of life; urinary control, erectile function and bowel function are the primary concerns. For this reason, we believe in having a thorough discussion with you to weigh the risks and benefits of each option.
Active Surveillance: Some forms of the disease may grow so slowly that they don’t pose a risk to your health and require no treatment at all. The objective for these indolent or slow cancers is to offer close surveillance instead of a curative intent, thereby avoiding the problems associated with treatment. Should the cancer show signs of progression, intervention is offered while the cancer is still curable; there is significant progression in only 27% of these indolent cancers. This may also be a good choice for a man with a longer life expectancy who has a low-risk tumor.
Radiation Therapy: There are two types: interstitial prostate brachytherapy and external beam radiation therapy. With interstitial prostate brachytherapy, small radioactive “seeds” are planted in the prostate. With external beam radiation therapy, the prostate is treated from externally with a beam of radiation. The advantage of radiation therapy is that it is less invasive than surgery. Urinary control may be affected less often after radiation than with radical prostatectomy; however, bowel function can be adversely affected after radiation but not so for surgery. For very aggressive diseases, surgery followed by radiation therapy may be the best chance for a cure. However, one disadvantage of radiation therapy is that surgery cannot be performed afterwards if there is a recurrence.
Surgery: A radical prostatectomy is the standard of care for removal of the entire prostate and accessory glands. This surgery offers the man with cancer that has not spread outside the prostate an excellent chance of cure of his disease; depending on the aggressiveness of cancer, the cure rate may be as high as 95%. The most common side effects are erectile dysfunction and impaired urinary control. The chance of having erectile dysfunction depends on a man’s age and health, his sexual function before treatment and the stage of the cancer. Even if erectile dysfunction does occur after surgery, erections may return to normal over time, and can be improved on with medical therapy. While many men experience some form of urinary incontinence following prostate cancer treatment, the vast majority do regain their continence within a year. We can also recommend physiotherapy to assist with urinary function recovery, or pre-operatively to improve the after-surgery outcomes.
Hormone Therapy:This involves either stopping your body from producing the male sex hormone testosterone which stimulates the growth of prostate cancer cells, or blocking testosterone from getting into the cancer cells. Sometimes a combination of two drugs is used to achieve both effects. Hormonal therapy is offered to men who choose not to have, or who cannot be treated with, curative therapies.
--
1. Aiken WD, Tulloch T, Freeman V, Bennett F, Coard K, Panton B et al. Differences in patient characteristics in black men with prostate cancer from Jamaica and Chicago. In: Proc Am Soc Clin Oncol 2003; 22: (abstr 1764).
2. Blake G, Hanchard B, Mitchell K, Waugh N, Wolff C, Samuels E. Jamaica Cancer Mortality Statistics, 1999. West Indian Med J 2002; 51: 64−7
Bladder Cancer
Bladder cancer is the fourth most common cancer in men and the eighth most common cancer in women. It typically occurs over the age of 55, but can also affect younger patients. The first warning sign may be blood in the urine (hematuria), which alarms many patients and causes them to seek an early Urological consult. Therefore, most bladder cancers are diagnosed early and are curable. Blood in the urine should never be ignored. Other symptoms include painful urination, frequent urination, and pelvic pain. Smoking is attributed to 50% of bladder cancers. Other risk factors include workplace chemicals, family history, and cancer treatments such as chemotherapy and radiation therapy.
Bladder cancer is diagnosed by the following tests:
Treatment choice is determined by the stage and grade of the tumor, where it is located, whether it has spread, and your general health and age. Options include Surgery, Chemotherapy, Radiation therapy, or a combination of those. We will help you to make the most informed decision.
Bladder cancer is diagnosed by the following tests:
- Urine tests (cytology): This test checks for cancerous cells in the urine
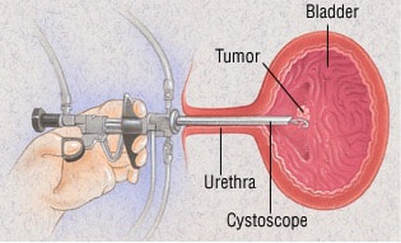
- Cystoscopy: This test evaluates the bladder for any abnormalities. A small camera is inserted into the urethra to visualize your bladder and urethra. This will allow us to identify any abnormal findings, such as stones, growths (cancers), enlarged prostates and foreign bodies as the cause of your hematuria. This procedure can be performed in office; it is completely painless, does not require you to be put to sleep, and is offered as an out-patient basis (you go home right afterwards).
- Biopsy: A sample of bladder tissue is taken during the cystoscopy. A pathologist will grade the bladder tissues samples, which then determines treatment options.
- Imaging: This is usually a CT scan to allow us to see the entire urinary tract and surrounding tissues.
Treatment choice is determined by the stage and grade of the tumor, where it is located, whether it has spread, and your general health and age. Options include Surgery, Chemotherapy, Radiation therapy, or a combination of those. We will help you to make the most informed decision.
- TURBT (transurethral resection of bladder tumor): This surgery is often used in early stage bladder cancers, before it invades the muscular lining of the bladder. An electrosurgical loop is used through a cystoscope in your bladder, under general anaesthesia. The loop removes all visible tumor. In early stage disease, this most often represents a cure.
- Radical Cystectomy: This is surgery to remove the entire bladder. It is reserved for invasive bladder cancer (involving the muscular layer of the bladder), or when other therapies have not been successful. Risks include erectile dysfunction and infertility for men, and premature menopause for women. Your bladder is then replaced with one of the following options:
- Urinary Conduit: This is the most common type of diversion where a segment of the intestine is used to create a connection from the kidneys to the outside of the body through an opening in the abdominal wall. Your urine empties continuously into a bag which you wear on your abdomen, under your clothes. This is the simplest procedure, associated with the lowest complication rates. However, some patients do not like the external appearance.
- Contino-cutaneous urinary diversion: An internal pouch is created from the intestines and urine is diverted and collects here. You empty the pouch a few times a day at your convenience using a catheter. There is a one-way valve to keep the urine inside the pouch. There is no external appliance and you remain dry of urine; it is the most convenient approach.
- Neobladder (new bladder): A segment of the intestine is harvested and used to create a new bladder. This procedure allows you to urinate in a more normal fashion, via your urethra, as you normally would have before your bladder was removed. The biggest advantage is continence, or control of your urine. The surgery is also more complex and patients have to re-learn how to urinate. You may also need to use a catheter to drain all the urine from the new bladder.
- Chemotherapy: This is an option for advanced bladder cancer. It usually involves two or more drugs to kill cancer cells. Drugs are injected into a vein in your arm (intravenously). It may be administered before and/or after surgery.
- Radiation Therapy: This can be used in combination with chemotherapy in patients with advanced bladder cancer. Radiation beams are delivered from a machine, precisely aimed at the cancer.
- In patients not fit for, or not desirous of, radical cystectomy, TURBT may be combined with chemotherapy and radiation to achieve similar results as surgery. Not all cases are candidates for this bladder sparing approach.
Kidney Cancer
Kidneys are two bean shaped organs that clean the blood of waste, which end up in your urine. Kidney cancer generally forms in the lining of the tubes that filter the blood inside the kidneys. Kidney cancer is among the top ten most common cancers in both men and women, and is the most dangerous of urological cancers. Most cases are detected these days incidentally, that is, when tests ordered for another problem detect a kidney mass. Therefore, most cases are detected at an early stage, when the cure/ survival rates are very high.
Risk factors that can increase your chance of kidney cancer include:
Symptoms of kidney cancer include:
The diagnosis of kidney cancer will include a complete medical history, physical exam and imaging (CT scan). In some situations a biopsy may be recommended, but most often surgery is performed and then the tumor is examined by a pathologist. Staging the tumor will show the extent of the disease and determine next steps.
Treatment options most often include surgery. This can be offered via laparoscopic (‘keyhole’) surgery, or an open procedure if the tumor is large. Targeted therapy (medication), and chemotherapy may be included in advanced cases.
Types of treatments include:
We will develop a customized treatment plan that will provide the most cutting-edge therapy with the best possible outcome. Less-invasive surgery (‘keyhole’ surgery) results in quicker recovery and fewer complications. Your treatment will be determined by your age, health, size, and location of your tumor. We will guide you through all of the available options; your health is our main concern.
Risk factors that can increase your chance of kidney cancer include:
- Smoking
- Family history
- Obesity
- Race – blacks have a slightly higher risk
- Sex – Men have about twice the risk
- High blood pressure
- Exposure to workplace chemicals
- Long-term dialysis
- Genetic disorders such as von Hippel-Lindau disease
Symptoms of kidney cancer include:
- Blood in the urine (hematuria)
- Lump in the abdomen or side
- Weight loss without trying
- Pain in your side, flank, or lower back that won’t go away
- Fatigue
- Fever
- Swelling in your ankles or legs
The diagnosis of kidney cancer will include a complete medical history, physical exam and imaging (CT scan). In some situations a biopsy may be recommended, but most often surgery is performed and then the tumor is examined by a pathologist. Staging the tumor will show the extent of the disease and determine next steps.
Treatment options most often include surgery. This can be offered via laparoscopic (‘keyhole’) surgery, or an open procedure if the tumor is large. Targeted therapy (medication), and chemotherapy may be included in advanced cases.
Types of treatments include:
- Radical nephrectomy is the removal of the whole kidney.
- Partial nephrectomy is removal of only the part of the kidney that contains the tumor. This is appropriate for early stage disease.
- Active surveillance involves delaying treatment and monitoring the tumor.
- Chemotherapy is utilized in more advanced cases.
We will develop a customized treatment plan that will provide the most cutting-edge therapy with the best possible outcome. Less-invasive surgery (‘keyhole’ surgery) results in quicker recovery and fewer complications. Your treatment will be determined by your age, health, size, and location of your tumor. We will guide you through all of the available options; your health is our main concern.
Testicular Cancer
Testicular cancer is very rare, especially in Jamaica. However, it is the most common cancer worldwide in men between the ages of 15 to 35. If detected early, it is curable in the majority of cases. Although the cause is unknown, the following risk factors have been found to be associated with the disease:
Most testicular cancer is found during a self-exam or at a physical with your doctor. It is recommended that you do monthly self-exams of your testes so that you will immediately notice any changes with your body. Symptoms may include:
If you or your doctor find a suspicious lump, blood tests are performed to identify tumor markers. Ultrasound, CT scan, chest x-ray, and MRI may be ordered as well. We treat your referral with the utmost of urgency. If a diagnosis is confirmed, it is important to stage the cancer in order to develop the best treatment plan.
Treatment for testicular cancer is determined by the stage. If you have early cancer, surgery to remove the testicle is the gold standard of treatment. This usually cures the cancer. This will be performed under general anesthesia. A schedule of follow-up appointments and scans will be set to make sure the cancer has not returned.
If you have more advanced cancer, you will need surgery to remove the affected testicle as well as the abdominal lymph nodes.
Chemotherapy or radiation may be needed for advanced stages of the disease as well; these modalities of treatment can cause permanent infertility. It is important to us to consider your fertility during this process. You may wish to store your sperm in a sperm bank if you plan on having children in the future. The majority of cancer is found in only one testicle; the other one will work fine to produce sex hormones (testosterone) and sperm. We will walk you through the best treatment options for you.
- Undescended testicle
- Family history of testicular cancer
- Genetic condition known as Klinefelter’s Syndrome
- HIV
Most testicular cancer is found during a self-exam or at a physical with your doctor. It is recommended that you do monthly self-exams of your testes so that you will immediately notice any changes with your body. Symptoms may include:
- Firm lump in your scrotum
- Swelling or enlarged testicle
- Pain or soreness in the testicle
If you or your doctor find a suspicious lump, blood tests are performed to identify tumor markers. Ultrasound, CT scan, chest x-ray, and MRI may be ordered as well. We treat your referral with the utmost of urgency. If a diagnosis is confirmed, it is important to stage the cancer in order to develop the best treatment plan.
Treatment for testicular cancer is determined by the stage. If you have early cancer, surgery to remove the testicle is the gold standard of treatment. This usually cures the cancer. This will be performed under general anesthesia. A schedule of follow-up appointments and scans will be set to make sure the cancer has not returned.
If you have more advanced cancer, you will need surgery to remove the affected testicle as well as the abdominal lymph nodes.
Chemotherapy or radiation may be needed for advanced stages of the disease as well; these modalities of treatment can cause permanent infertility. It is important to us to consider your fertility during this process. You may wish to store your sperm in a sperm bank if you plan on having children in the future. The majority of cancer is found in only one testicle; the other one will work fine to produce sex hormones (testosterone) and sperm. We will walk you through the best treatment options for you.